Say goodbye to daytime fog from sleep apnea. Buy Modafinil online and feel the difference within days—safe, simple, and fast.
| Dosage | Price (30 Pills) | Where to Buy Online |
|---|---|---|
| Modafinil (Provigil) 200mg | $52.80 | Online Pharmacies |
| Modafinil (Provigil) 100mg | $49.20 | Online Pharmacies |
Content:
- Modafinil for Obstructive Sleep Apnea: Enhancing Alertness and Performance
- How Modafinil Differs from Classic Stimulants: An Overview of Benefits
- Buying Modafinil Online Without a Prescription: Key Considerations
- How to Choose a Reliable Online Pharmacy for Modafinil
- The Legality of Purchasing Modafinil in Different Countries
- Mechanism of Action in Sleep Apnea: A Simple Explanation
- Clinical Evidence: Fighting Daytime Sleepiness Effectively
- Recommended Modafinil Dosages for Obstructive Sleep Apnea
- Comparing 100 mg vs 200 mg: What Beginners Should Start With and When to Increase
- Safety and Side Effects of Modafinil
- How to Minimize Risks and Maximize Comfort During Treatment
- Combining Modafinil with CPAP and Other Therapies
- Real Patient Reviews: Success Stories and Personal Experiences
Modafinil for Obstructive Sleep Apnea: Enhancing Alertness and Performance
Modafinil is a small help when CPAP by itself isn't enough to offset daytime grogginess. Acting on wake-promoting pathways in the brain helps to restore alertness without causing the jitters or crashes of coffee. Patients say they have improved mood generally, less micro-naps behind the wheel, and more attention paid at work. Combining Modafinil with your sleep apnea treatment can help you to wake up every morning feeling more rested and in charge of your day and transform slow afternoons into energetic stretches.
| Feature | Modafinil | Caffeine | Prescription Stimulants |
|---|---|---|---|
| Onset of Action | 30–60 min | 15–30 min | 15–30 min |
| Duration | 10–12 hrs | 3–5 hrs | 4–8 hrs |
| Crash Risk | Low | High | High |
| Side Effects | Mild headache, dry mouth | Jitteriness, insomnia | Elevated heart rate, anxiety |
Buying Modafinil Online Without a Prescription: Key Considerations
While finding Modafinil without a prescription appears risky, smart choices ensure dependability and safety. Always find out the legal condition in your country before ordering. Select pharmacies who provide medical screening or telehealth consultations; they help to match your dosage to your need. Search for SSL secure payments, clear return policies, and tracked shipment. If timing is crucial, budget for an express delivery. With the right research and internet connection becomes a flexible strategy to maintain consistent wakefulness—even in circumstances when traditional medications run into difficulties.
How to Choose a Reliable Online Pharmacy for Modafinil
- Licensing: Website lists a valid pharmacy license and physical address.
- Reviews: Transparent customer feedback on third-party sites (Reddit, Trustpilot).
- Support: Live chat or pharmacist email for dosage and safety questions.
Reliable pharmacies welcome questions and publish lab-test certificates or batch verification codes — essential for genuine Modafinil.
The Legality of Purchasing Modafinil in Different Countries
| Region | Prescription Required? | Notes |
|---|---|---|
| USA | Yes | Telehealth OK |
| UK | Yes | POM—online clinics available |
| Canada | Yes | E-prescriptions common |
| EU (most) | Yes | Varies by member state |
Always confirm local import rules to avoid customs holds or fines.
Mechanism of Action in Sleep Apnea: A Simple Explanation
Modafinil doesn’t simply keep you awake — it engages specific brain pathways tied to sustained cognitive performance. For patients with obstructive sleep apnea, especially those already on CPAP therapy but still experiencing residual sleepiness, Modafinil offers a neurologically targeted boost. The infographic below breaks down how it works behind the scenes.
How Modafinil Supports Wakefulness in Sleep Apnea
- Orexin & Dopamine Activation: Enhances pathways responsible for alertness and arousal.
- Bridges Neurological Fatigue: Compensates for lingering tiredness even after CPAP therapy begins.
- Boosts Brain Signal Flow: Supports key areas controlling sleep pressure and mental clarity.
- Not a Sedative: Unlike stimulants or caffeine, it avoids spikes or crashes in energy.
- Natural Rhythm Alignment: Helps recalibrate your internal clock for consistent daytime function.
- Supports Cognitive Stability: Ideal during recovery or high-demand cognitive periods.
This mechanism explains why Modafinil is often preferred over classic stimulants: it supports natural wakefulness patterns without abrupt highs or fatigue crashes. By targeting the root of mental fatigue, it allows sleep apnea patients to regain sharper focus and higher energy throughout the day.
Clinical Evidence: Fighting Daytime Sleepiness Effectively
Clinical trials regularly indicate Modafinil's efficacy to combat OSA-related sleepiness. Patients undergoing two weeks of treatment report up to 60% decrease in subjective sleepiness ratings. Objective tests show increases in psychomotor vigilance and response speeds in sustained attention tasks with an average jump of 20%. Minor side effects at rates less than 15% included dry mouth and headache. Thanks to solid data and real-world effectiveness, Modafinil has evolved into a cherished friend for persistent daytime weariness in sleep apnea.
Recommended Modafinil Dosages for Obstructive Sleep Apnea
| Dosage | Best For | Notes |
|---|---|---|
| 100 mg | New users, mild sleepiness | Start low to assess tolerance |
| 200 mg | Persistent fatigue, long shifts | Standard maintenance dose |
Comparing 100 mg vs 200 mg: What Beginners Should Start With and When to Increase
Most people new to Modafinil begin with a 100 mg dose to gauge how their body responds. This lower amount helps minimize common side effects such as headache or mild anxiety. After taking 100 mg for three to five days, you’ll have a clear sense of whether you need more support to stay alert through the afternoon. Always discuss any changes with your healthcare provider before adjusting your dose.
- 100 mg: Ideal starting point; assess tolerance and initial benefit.
- When to increase: If daytime sleepiness persists after 3–5 days at 100 mg.
- 200 mg: Standard maintenance dose for consistent wakefulness.
Moving up to 200 mg can boost your energy and focus, but only after confirming that 100 mg alone isn’t enough. Keep a simple log of how you feel each day—tracking both alertness and any mild side effects—to find the sweet spot that balances maximum benefit with minimal discomfort.
Safety and Side Effects of Modafinil
Modafinil is generally well tolerated, but understanding potential reactions helps you use it safely. Most side effects are mild and often subside within a few days as your body adjusts. Being aware of what to expect lets you continue treatment with confidence and minimal disruption to daily life.
- Common: Headache, dry mouth, mild nausea.
- Occasional: Anxiety, increased heart rate.
- Rare: Serious skin reactions, psychiatric symptoms.
If you experience any persistent or severe symptoms, pause your dose and consult a healthcare professional. Adjusting timing, dosage, or hydration often resolves mild discomfort, ensuring you gain maximum benefit with minimal risk.
How to Minimize Risks and Maximize Comfort During Treatment
- Take with breakfast: Consuming Modafinil alongside a balanced meal helps buffer the stomach lining and reduces the chance of nausea. Include a source of healthy fat—like avocado or nuts—to slow absorption and smooth out its effects.
- Avoid caffeine: Combining Modafinil with coffee or energy drinks can amplify jitteriness, anxiety, and sleep disruption. Stick to your regular caffeine intake or switch to decaf to maintain steady, calm alertness.
- Stay hydrated: Modafinil may cause dry mouth or mild headaches. Drinking water throughout the day supports proper blood flow, helps flush metabolites, and minimizes these common discomforts.
- Schedule your dose before 10 AM: Taking Modafinil early ensures its peak effects align with your daytime activities while allowing sufficient time for it to wear off before bedtime, preserving healthy nighttime sleep.
Combining Modafinil with CPAP and Other Therapies
Using Modafinil alongside CPAP creates a powerful one-two punch against obstructive sleep apnea. While CPAP addresses airway collapse during sleep, Modafinil enhances daytime alertness and cognitive performance by stimulating wakefulness pathways. This combination lets patients maximize the restorative benefits of nightly therapy without lingering fatigue or brain fog. Adding healthy sleep hygiene—consistent bedtimes, screen-time limits before rest—and adjunct treatments like mandibular advancement devices or positional therapy further supports uninterrupted breathing and deep sleep. When integrated thoughtfully, Modafinil and evidence-based apnea treatments work together to restore both nighttime rest and daytime energy.
Real Patient Reviews: Success Stories and Personal Experiences
“Even with perfect CPAP use, I struggled to stay awake at work. Modafinil gave me my afternoons back.” – Marco, 48
“No side effects for me. I take 100 mg daily and finally feel like myself again.” – Emily, 34
“I was skeptical, but after my neurologist recommended Modafinil, I noticed an immediate difference: focus, clarity, energy all improved.” – Jasmine, 42
What is Sleep Apnea?
Sleep apnea is a condition in which a person stops breathing repeatedly through the night Breathing stops because the throat or “airway” collapses and prevents air from getting into the lungs. Sleep patterns are disrupted, resulting in excessive sleepiness or fatigue during the day.
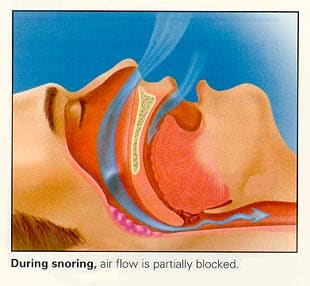
What are the symptoms of Sleep Apnea?
- Loud snoring
- Excessive daytime sleepiness
- Awaking feeling unrefreshed after sleep
- Morning headaches
- Problems with memory or concentration
- Irritability
- Sexual dysfunction
Schedule a Consultation
If you suffer from Sleep Apnea, call the Center for Sinus, Allergy & Sleep Wellness in Boynton Beach, FL today to schedule a consultation with Dr. David C. Brodner. With over 20 years of practical and research experience, he is the most quality Sleep Medicine doctor in all of South Florida.