
Fun Facts About Snoring
You are not alone! Did you know that 20% of all adults suffer from chronic snoring and almost half snore at least occasionally? Snoring is the harsh sound created by vibrations of the soft tissues of the throat – mainly the soft palate and uvula, but also implicated are the tonsils and tongue.
Frequently there is more than one anatomical area involved, which is the reason a multilevel approach is a correct method to manage your snoring and Obstructive Sleep Apnea. Dr. Brodner can help you with providing snoring treatment in Boynton Beach. Dial 561.735.8750 today to schedule your consultation and learn more!
Patient Testimonial
"Had chronic sinus issues for years and decided to finally get checked out. Dr Brodner and his team methodically determined that I was a good candidate for the balloon sinuplasty procedure. They explained all the details and assured me of the benefits. After four weeks I have never felt better, can breath through my nose clearly for the first time that I can remember and my snoring and post nasal drip have significantly diminished. Follow ups have been great and I would highly recommend this team for anyone considering this type of procedure."
- S.B.
What causes Snoring?
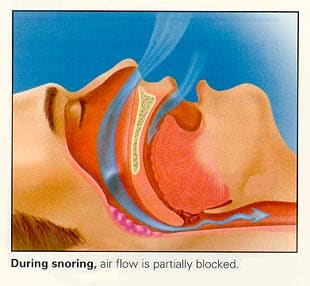
The soft palate and uvula elongate. This allows the relaxed tongue to partially block the airway. The uvula and soft palate vibrate during inhalation, creating the snoring sound.
How is Snoring diagnosed?
At your first visit, he will assess your sinonasal and upper airways to determine which anatomic levels are involved in your snoring. Utilizing the latest equipment and techniques, including flexible fiberoptic endoscopy – a tiny camera that fully visualizes the inside of your throat – Dr. Brodner will localize the sites of your obstruction.
Finally, you will be sent for a sleep study (polysomnogram) to ensure your snoring does not represent the more serious medical problem, Obstructive Sleep Apnea.
Dr. Brodner will personally read your sleep study and, if the data indicates the absence of Obstructive Sleep Apnea, he will notify you of the various treatment options available to improve your disruptive snoring.
These may include:
- Lifestyle Modifications.
- A minimally invasive in-office procedure such as Coblation Snoring treatment.
- Treating Sinonasal problems like allergies, polyps, or a deviated septum.
Lifestyle modifications involve avoidance of the many factors that exacerbate the loudness and intensity of your snoring:
- Weight loss is recommended to decrease bulky tissues lining the throat, due in part to excess body weight, which worsens snoring by providing more vibratory material.
- Do not sleep supine (on your back) – it promotes snoring as gravity positions the uvula and soft palate downward, enabling more movement.
- Finally, shun anything that causes a deeper sleep – alcohol, sedative medications, or sleep deprivation.
These all exacerbate both snoring and sleep apnea by making you less arousable, less likely to switch body positions, and have decreased muscle tone which leads to increased vibrations.
Dr. Brodner may determine that management of your nose and/or sinuses is pivotal to controlling your snoring. Nasal obstruction, with subsequent mouth breathing, worsens snoring by increasing the magnitude of soft tissue vibrations.
The passageway may be obstructed by swelling of the turbinates due to allergies, a septal deviation (crookedness of the middle divider in the nose), or nasal polyps. Medication and/or surgery to address these problems can improve the flow of air through the nasal passages, thus reducing troublesome snoring.
If your snoring keeps you up at night, call the Center for Sinus, Allergy and Sleep Wellness in Boynton Beach, FL today and sleep soundly once again!
What does normal sleep look like?
Normal Sleep is where the tongue is relaxed and falls back slightly but does not interfere with the airway.
Surgical Procedures for Snoring
If the nasal obstruction is not an issue, Dr. Brodner will determine if your anatomy is conducive to the surgical correction of the snoring. He offers the latest in-office minimally-invasive procedures:
- Injection Snoreplasty
- Pillar Implant
Both are performed in the office, under local anesthesia, with you awake.
The concept is to stiffen the palate tissues by creating a scar, which vibrates less and therefore decreases the intensity of your snoring. If your anatomy warrants a more aggressive approach, Dr. Brodner is experienced with minimally-invasive PEAK uvuloplasty reconstruction performed in the operating room under general anesthesia.

Why choose Dr. Brodner for your Snoring Treatment?
David C. Brodner, MD is a double Board-Certified Sleep Medicine specialist, which qualifies him with the expertise to perform a comprehensive Sleep Medicine and ENT examination and can provide you with effective snoring treatment in Boynton Beach.
Dr. Brodner has also lectured both locally and nationally on Sleep Apnea and CPAP therapy, services as Medical Director for Sleep Labs in Boca Raton, Lake Worth, and Deerfield Beach, and runs an Insomnia Management Clinic in Boynton Beach, Florida.
He also created a line of All-Natural Nutraceutical Sleep Aids to assist patients in seeking a more natural path towards sleep-wellness. Dr. Brodner established the Center for Sinus, Allergy, and Sleep Wellness in 2009 to offer the latest cutting-edge technology and techniques to patients from Wellington to Palm Beach, Jupiter to Delray Beach, and beyond.
Call Dr. Brodner for Snoring Treatment in Boynton Beach!
If you are interested in learning more about Dr. Brodner's snoring treatment in Boynton Beach, FL, please contact us for a consultation at 561.735.8750 or fill out our contact us form below. We will discuss your needs and concerns, and determine your best course of action.


